Junior doctor contracts
Gauging public support for strike action
If junior doctors vote to proceed with the strike, which from all accounts looks likely, there will be three independent days of walk-outs that will hit the NHS as it ramps up to the busy December period.A month ago, Opinium in partnership with the Observer polled the UK public on their level of support for junior doctors and Jeremy Hunt. Just as 20,000 junior doctors took to the streets of Whitehall to protest the changes to their contracts, our research showed that 41% of the UK public would find it justifiable for junior doctors to take strike action.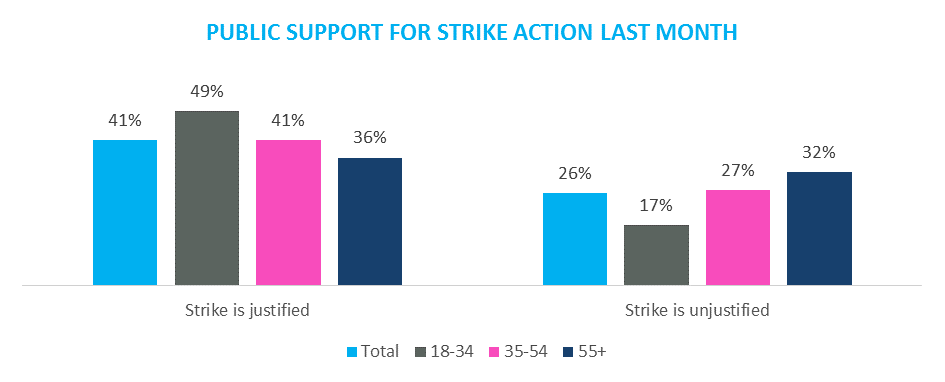 Much has happened since then. On 3 November, Jeremy Hunt made the shock declaration that he would offer junior doctors an 11% rise in basic pay in compensation for changes to their working hours. The move was a brilliant piece of political manoeuvring with many spectators pointing out that it still did not compensate for the estimated 20% – 30% loss in out-of-hours pay expected to hit doctors. On 12 November, the BMA followed the Health Secretary by announcing the dates for strike action.We took this as an opportunity to review public support for junior doctors and asked our nationally representative sample of 2,000 UK adults whether they approved or disapproved of the action.41% OF THE UK PUBLIC APPROVE OF THE PROPOSED STRIKE ACTION There is good and bad news for both the BMA and the Health Secretary emerging from our results. For the BMA, the good news is that the level of support for their cause has not diminished one iota. In fact, support has intensified among that group with 19% saying they strongly approve of strike action compared to 11% a month ago.The bad news is that disapproval of strike action has increased compared to a month ago from 26% to 39%. This is good news for the Health Secretary, as it suggests that as the public has come closer to facing the realities of a strike, sentiments have hardened against junior doctors in some pockets of the population.So, where has this sudden opposition come from?It appears to be driven mainly by an increase in Conservative voter opposition to the strikes, which has increased dramatically since we last asked the question. Indeed, a full 60% of those who voted Conservative earlier this year oppose strike action from junior doctors. It is not only Tory voters who are driving this opposition. We also see an increase in opposition from a wide range of voters (though the next highest increase after the Tories are admittedly UKIP). For example, there has been an increase in opposition among Labour voters from 13% to 23% over the past month. If we look at demographic data, we can start to hypothesise about other factors driving opposition: Support for junior doctors was previously highest amongst 18-34 year olds. In the past month, their support has waned and their opposition increased. Why should this be the case?There are three possible reasons. The first reason could be that this generation has grown up with a prevailing narrative that demonises almost all unionised action and as a result this increase in opposition, where there was once support, represents a Pavlovian response. The second reason could be that these individuals, more likely to be early-in-career, have seen headlines around an 11% increase in pay and have unfavourably compared their lot to that of junior doctors. The third reason (and most likely, in my opinion) is quite simple and it is that the vast majority of 18-34 year olds rarely use hospitals for routine check-ups (though there are obvious exceptions). For the most part, their use of healthcare services tends to be acute, seeking help in cases of emergency. And so the prospect that A&E Departments might be worse-off for two days in December (three if you only read the headlines) can start to generate real concerns over the quality of care.But whatever the case may be, the lesson to be drawn from our data is that while opposition may have strengthened and coalesced in the past 30 days, there is overall support for junior doctors to go on strike. The BMA should take heart from that, no matter the result come 5pm today.A FORK IN THE ROADEarlier, I described this dispute over contracts as a war. Some may find that phrasing overly dramatic, but I think it is an apt phrase to describe a dispute that has been bubbling under the surface of the NHS since 2012. Both sides have emphasised the importance of this dispute in outlining the future of the health service in the UK for years to come, albeit it for different reasons. And both are absolutely correct. The weekend mortality rates that the Department of Health have placed at the heart of this debate do demonstrate that there is room for improvement in patient outcomes. And while it needs to be emphasised that Sir Bruce Keogh’s review did not categorically state that lower levels of service were the cause of higher mortality rates (it only hypothesised), it would be fair to say that service delivery at weekends could be better designed to provide more equal coverage throughout the week.However, a seven-day health service cannot be fully delivered without an increase in the multidisciplinary services around Emergency Departments, which will require certain specialties to work more hours over the course of the week. But to increase working hours without an increase in resources ? both in terms of funding and personnel ? is short-sighted and could set the NHS down a perilous and ruinous path. Indeed, the GMC reported in September that requests for certificates of professional status ? an indicator that a doctor is looking to move overseas for work ? had increased by almost 22 times the normal number.It costs an average of £300,000 to train a doctor to Registrar level and the GMC receives an average of 3,000 requests for certificates each year. Even if half of those requests lead to a junior doctor leaving the UK to work abroad, the unrecoverable cost of training those doctors will be almost £500 million ? the equivalent to a quarter of the forecasted NHS deficit for this year. These figures should serve as a sobering reminder that should negotiations continue to falter, there could be a dramatic economic cost to Jeremy Hunt?s proposals. But perhaps that should not be our focus of concern.The biggest issue that our society contends with when it comes to healthcare is the politicisation that occurs as a result of it being nationalised and tax-payer funded. Economic arguments and centre-ground winning policies dominate our conversation about healthcare. But the fact is that junior doctors are human beings, not robots. Like everyone else, they require food, water, shelter, sleep and time away from work. Their days are spent churning through a relentless caseload of patients, struggling with reduced resources to deliver the best care possible and, for many, dealing with the psychological stresses that come from the inevitable fact that some patients never recuperate. And at the end of the day, these junior doctors ? many of whom are not ?junior? at all ? must study to maintain their ability to practice and advance in their training.Perhaps it?s time for us to shift our perspective of the NHS away from institutionalised and politicised arguments and recognise it for what it is. An organisation that survives based on the dedicated work of human beings struggling to make other human beings better.James leads the Healthcare practice at Opinium Research and has a strong interest in healthcare, pharmaceuticals and medical equipment. If you?d like to know more about our Healthcare practice or our research in this area, please get in touch.
Much has happened since then. On 3 November, Jeremy Hunt made the shock declaration that he would offer junior doctors an 11% rise in basic pay in compensation for changes to their working hours. The move was a brilliant piece of political manoeuvring with many spectators pointing out that it still did not compensate for the estimated 20% – 30% loss in out-of-hours pay expected to hit doctors. On 12 November, the BMA followed the Health Secretary by announcing the dates for strike action.We took this as an opportunity to review public support for junior doctors and asked our nationally representative sample of 2,000 UK adults whether they approved or disapproved of the action.41% OF THE UK PUBLIC APPROVE OF THE PROPOSED STRIKE ACTION There is good and bad news for both the BMA and the Health Secretary emerging from our results. For the BMA, the good news is that the level of support for their cause has not diminished one iota. In fact, support has intensified among that group with 19% saying they strongly approve of strike action compared to 11% a month ago.The bad news is that disapproval of strike action has increased compared to a month ago from 26% to 39%. This is good news for the Health Secretary, as it suggests that as the public has come closer to facing the realities of a strike, sentiments have hardened against junior doctors in some pockets of the population.So, where has this sudden opposition come from?It appears to be driven mainly by an increase in Conservative voter opposition to the strikes, which has increased dramatically since we last asked the question. Indeed, a full 60% of those who voted Conservative earlier this year oppose strike action from junior doctors. It is not only Tory voters who are driving this opposition. We also see an increase in opposition from a wide range of voters (though the next highest increase after the Tories are admittedly UKIP). For example, there has been an increase in opposition among Labour voters from 13% to 23% over the past month. If we look at demographic data, we can start to hypothesise about other factors driving opposition: Support for junior doctors was previously highest amongst 18-34 year olds. In the past month, their support has waned and their opposition increased. Why should this be the case?There are three possible reasons. The first reason could be that this generation has grown up with a prevailing narrative that demonises almost all unionised action and as a result this increase in opposition, where there was once support, represents a Pavlovian response. The second reason could be that these individuals, more likely to be early-in-career, have seen headlines around an 11% increase in pay and have unfavourably compared their lot to that of junior doctors. The third reason (and most likely, in my opinion) is quite simple and it is that the vast majority of 18-34 year olds rarely use hospitals for routine check-ups (though there are obvious exceptions). For the most part, their use of healthcare services tends to be acute, seeking help in cases of emergency. And so the prospect that A&E Departments might be worse-off for two days in December (three if you only read the headlines) can start to generate real concerns over the quality of care.But whatever the case may be, the lesson to be drawn from our data is that while opposition may have strengthened and coalesced in the past 30 days, there is overall support for junior doctors to go on strike. The BMA should take heart from that, no matter the result come 5pm today.A FORK IN THE ROADEarlier, I described this dispute over contracts as a war. Some may find that phrasing overly dramatic, but I think it is an apt phrase to describe a dispute that has been bubbling under the surface of the NHS since 2012. Both sides have emphasised the importance of this dispute in outlining the future of the health service in the UK for years to come, albeit it for different reasons. And both are absolutely correct. The weekend mortality rates that the Department of Health have placed at the heart of this debate do demonstrate that there is room for improvement in patient outcomes. And while it needs to be emphasised that Sir Bruce Keogh’s review did not categorically state that lower levels of service were the cause of higher mortality rates (it only hypothesised), it would be fair to say that service delivery at weekends could be better designed to provide more equal coverage throughout the week.However, a seven-day health service cannot be fully delivered without an increase in the multidisciplinary services around Emergency Departments, which will require certain specialties to work more hours over the course of the week. But to increase working hours without an increase in resources ? both in terms of funding and personnel ? is short-sighted and could set the NHS down a perilous and ruinous path. Indeed, the GMC reported in September that requests for certificates of professional status ? an indicator that a doctor is looking to move overseas for work ? had increased by almost 22 times the normal number.It costs an average of £300,000 to train a doctor to Registrar level and the GMC receives an average of 3,000 requests for certificates each year. Even if half of those requests lead to a junior doctor leaving the UK to work abroad, the unrecoverable cost of training those doctors will be almost £500 million ? the equivalent to a quarter of the forecasted NHS deficit for this year. These figures should serve as a sobering reminder that should negotiations continue to falter, there could be a dramatic economic cost to Jeremy Hunt?s proposals. But perhaps that should not be our focus of concern.The biggest issue that our society contends with when it comes to healthcare is the politicisation that occurs as a result of it being nationalised and tax-payer funded. Economic arguments and centre-ground winning policies dominate our conversation about healthcare. But the fact is that junior doctors are human beings, not robots. Like everyone else, they require food, water, shelter, sleep and time away from work. Their days are spent churning through a relentless caseload of patients, struggling with reduced resources to deliver the best care possible and, for many, dealing with the psychological stresses that come from the inevitable fact that some patients never recuperate. And at the end of the day, these junior doctors ? many of whom are not ?junior? at all ? must study to maintain their ability to practice and advance in their training.Perhaps it?s time for us to shift our perspective of the NHS away from institutionalised and politicised arguments and recognise it for what it is. An organisation that survives based on the dedicated work of human beings struggling to make other human beings better.James leads the Healthcare practice at Opinium Research and has a strong interest in healthcare, pharmaceuticals and medical equipment. If you?d like to know more about our Healthcare practice or our research in this area, please get in touch.




